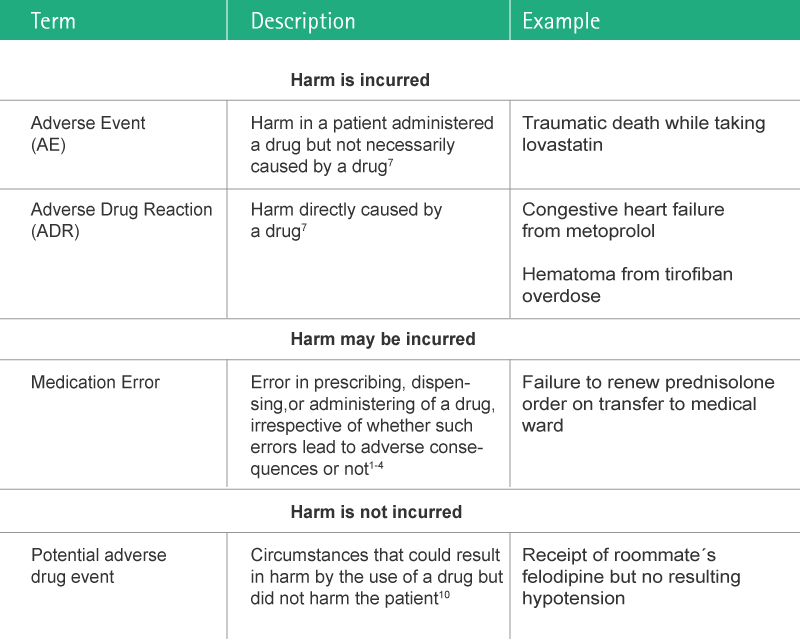
Medication Error
Medication error is an error in prescribing, dispensing or administering of a drug, irrespective of whether such errors lead to adverse consequences or not.1,2
Did you know?

(1) James JT. A new, evidence-based estimate of patient harms associated with hospital care. J Patient Saf. 2013 Sep;9(3):122-8
(2) Valentin A, Capuzzo M, Guidet B, Moreno RP, Dolanski L, Bauer P, Metnitz PG; Research Group on Quality Improvement of European Society of Intensive Care Medicine; Sentinel Events Evaluation Study Investigators. (2006) Patient safety in intensive care: results from the multinational Sentinel Events Evaluation (SEE) study. Intensive Care Med; 32(10): 1591-8
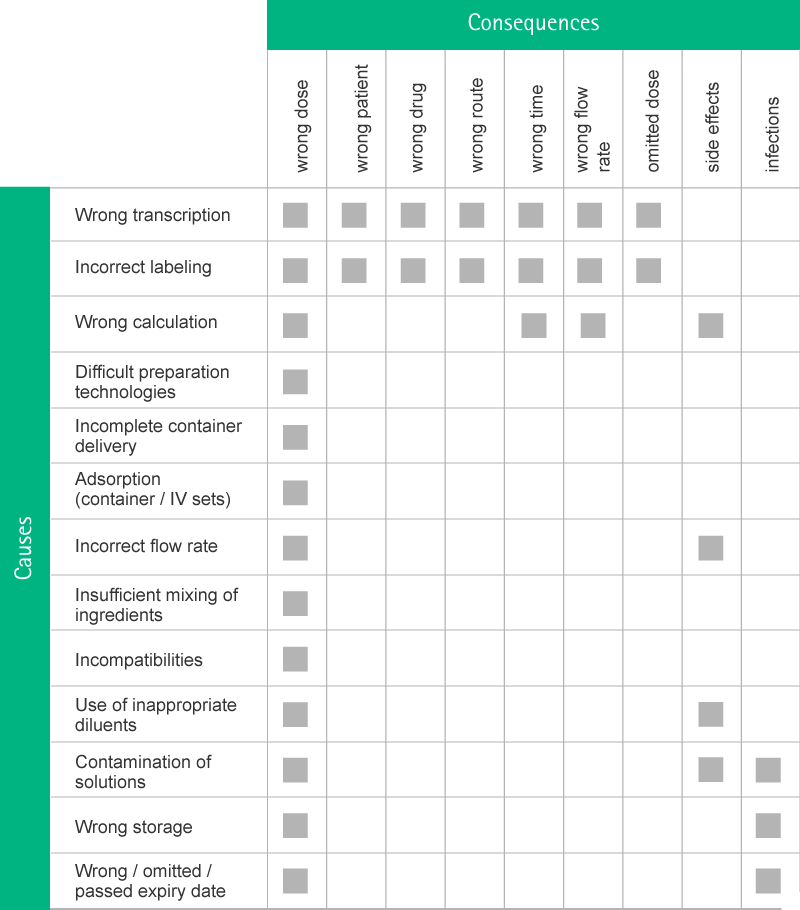
Causes
Parenteral medication errors are a serious safety problem in Intensive Care Units (ICU) and are recognized as a high priority health care issue across national borders, different ICU-settings and health care systems.1,2,5 Errors have been shown to be associated with additional morbidity and mortality in an already critically ill population.3,4
The majority of medication errors do not occur in emergency situations but while performing routine clinical tasks.5 The source of these errors can lie at any stage of the process from the initial prescription of an infusion to its administration.11 This is a complex process12 and can lead to a wide range of different errors.13-18
One of the reasons adverse events are so common is that clinicians are human, and thus prone to error. The seminal study by Wilson et al. found that human error was a significant factor. The majority (81%) of adverse events in their study were associated with one or more human factors, such as lack of knowledge, care or attention.19 Of the events that were considered highly preventable, less than 1% were not associated with human error.19
There are main causes which increase the incidence of Medication Error5:
- nurse’s workload (patient to nurse ratio, occupancy rate, ratio of beds per nurses
- size of unit (complexity of organization)
- look alike / sound alike drug labels and names.
Health Consequences
Since the early 70s more and more studies of the quantity of parenteral medication errors have been published.4 The National Patient Safety Agency in the United Kingdom has compiled figures showing the type of medication error incidents that actually occur. More than 14,000 injectable medicine incident reports during 18 months were evaluated.25 It was found that in more than 4,107 cases (28.9% of total) the most frequent medication error was wrong dose, strength or frequency of the prescribed drug.
Errors and irregularities in IV drug preparation can have a broad range of consequences ranging from harmless to serious to fatal. The severity depends on the drug in use and the specific factors of each individual case.
Financial Consequences
The financial costs of adverse events, in terms of additional treatment and extra days in hospitals, are considerable. For example, in Britain, the cost of preventable adverse events is £1 billion per annum in lost bed days alone.22 The wider costs of lost working time, disability benefits and further economic consequences are greater still.
The US Institute of Medicine report estimated that preventable medical errors result in total costs (including the expense of additional care caused by the errors, lost income, household productivity, and disability) of between $ 17 billion and $ 29 billion per year in US hospitals.32
Research in Australia showed that total costs of adverse events represent 15.7% of the total expenditure on direct hospital costs.33
Other significant damages associated with adverse events are the human ones: the harm suffered by the patient. Patients experiencing an adverse event are 4-7 times more likely to die than those who do not.33 Vincent et al. found that 19% of adverse events result in moderate physical impairment, 6% in permanent impairment and 8% in death.22
Potential Risk Associated Cost
A cost evaluation of the risk can be done by assigning costs to their related clinical treatment and resulting extended length of stay. The cost can be calculated using the average daily cost of the expected clinical treatment.30,31 The figure below shows the results of such a calculation for selected examples of complications.
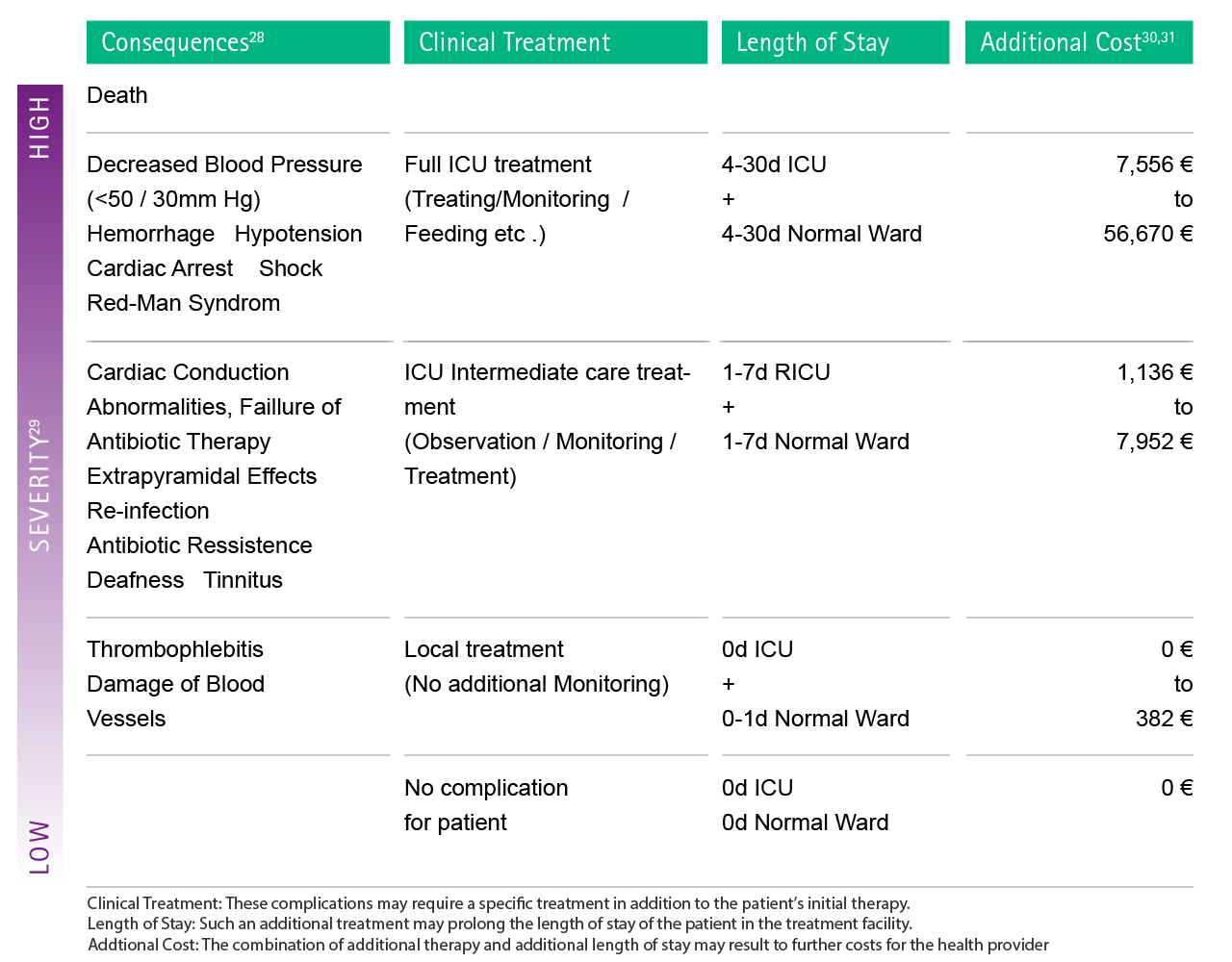
Fig. 3: Estimation of possible additional costs as a consequence of complications caused by medication error. In order to facilitate the attribution of each complication to the cost calculation, severity levels were introduced. RICU: Respiratory Intermediate Care Unit
Subsequently, in the case of severe complications which require full ICU treatment for diverse days of hospitalization, a hospital may save between 7,556 € and 56,670 € per single case.28-31
Preventive Strategies
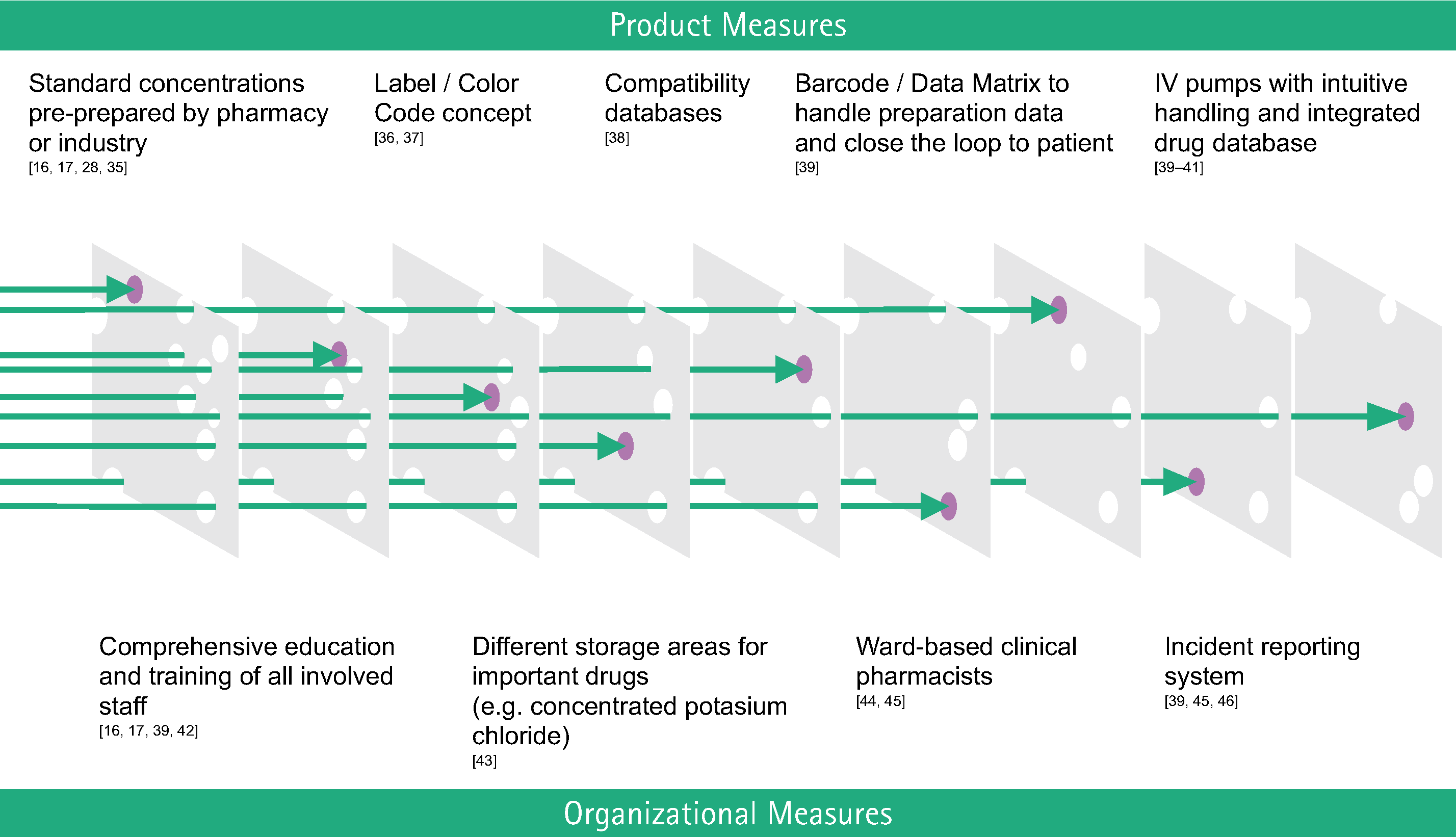
To prevent medication error and effectively ensure safe patient treatment it is important to combine product and organizational measures.
The more successive safety checks that are added, the safer the whole system becomes. Some concrete preventive strategies to implement in clinical routine are described in Figure below.
Moreover, it must be the aim of every employee in the healthcare sector, to ensure the 9 “Rights“.26,27
Highlight Safety Products
Scientific Evidence
1 Döring M, Brenner B, Handgretinger R, Hofbeck M, Kerst G. (2014) Inadvertent intravenous administration of maternal breast milk in a six-week-old infant: a case report and review oft he literature. BMC Res Notes; 7:17
2 Manias E, Kinney S, Cranswick N, Williams A, Borrott N. (2014) Interventions to reduce medication errors in pediatric intensive care. Ann Pharmacother; 48(10): 1313-31
3 JCAHO. (2014) Tubing misconnections - a persistent and potentially deadly occurrence. Joint Commission on Accreditation of Healthcare Organizations, USA. Sentinel Event Alert; 53: 1-3.
4 Simmons D, Symes L, Graves K. (2011) Tubing misconnections: normalization of deviance. Nutrition in Clinical Practice; 26(3): 286-293.
5 Valentin A, Capuzzo M, Guidet B, Moreno RP, Dolanski L, Bauer P, Metnitz PG; Research Group on Quality Improvement of European Society of Intensive Care Medicine; Sentinel Events Evaluation Study Investigators. (2006) Patient safety in intensive care: results from the multinational Sentinel Events Evaluation (SEE) study. Intensive Care Med; 32(10): 1591-8
6 Institute of Medicine (2007)
7 Edwards IR1, Aronson JK. (2000) Adverse drug reactions: definitions, diagnosis, and management. Lancet; 356(9237) :1255-9.
8 Bates DW, Cullen DJ, Laird N, Petersen LA, Small SD, Servi D, et al. (1995) Incidence of adverse drug events and potential adverse drug events. Implications for prevention. ADE Prevention Study Group. JAMA; 274(1): 29-34.
9 Gurwitz JH, Field TS, Avorn J, McCormick D, Jain S, Eckler M, et al. (2000) Incidence and preventability of adverse drug events in nursing homes. Am J Med; 109(2): 87-94.
10 Nebeker JR, Barach P, Samore MH. (2004) Clarifying adverse drug events: a clinician's guide to terminology, documentation, and reporting. Ann Intern Med;140(10):795-801.
11 McDowell S, Mt-Isa S, Ashby D (2010) Where errors occur in the preparation and administration of intravenous medicines: a systematic review and Bayesian analysis. Qual Saf Health Care; 19(4): 341-5
12 Fraind DB, Slagle JM, Tubbesing VA, Hughes SA, Weinger MB (2002) Reengineering intravenous drug and fluid administration processes in the operating room: step one: task analysis of existing processes. Anesthesiology; 97(1): 139-47.
13 Fahimi F, Ariapanah P, Faizi M, Shafaghi B, Namdar R, Ardakani MT (2008) Errors in preparation and administration of intravenous medications in the intensive care unit of a teaching hospital: an observational study. Aust Crit Care; 21(2): 110-6.
14 Ferner RE, Langford NJ, Anton C, Hutchings A, Bateman DN, Routledge PA (2001) Random and systematic medication errors in routine clinical practice: a multicentre study of infusions, using acetylcysteine as an example. Br J Clin Pharmacol; 52(5): 573-7.
15 Garnerin P, Pellet-Meier B, Chopard P, Perneger T, Bonnabry P (2007) Measuring human-error probabilities in drug preparation: a pilot simulation study. Eur J Clin Pharmacol; 63(8): 769-76
16 Parshuram CS, To T, Seto W, Trope A, Koren G, Laupacis A (2008) Systematic evaluation of errors occurring during the preparation of intravenous medication. CMAJ; 178(1): 42-8.
17 Cousins DH, Sabatier B, Begue D, Schmitt C, Hoppe-Tichy T (2005) Medication errors in intravenous drug preparation and administration: a multicentre audit in the UK, Germany and France. Qual Saf Health Care; 14(3): 190-5.
18 Cohen H, Robins ES, Mandrack M (2003) Getting to the root of medication errors: Survey results. Nursing; 33(9): 36-45.
19 Wilson RMcL, Harrison BT, Gibberd RW, Hamilton JD (1999) An analysis of the causes of adverse events from the Quality in Australian Health Care Study. Med J Aust; 170(9): 411-5.
20 Shane R. (2009) Current status of administration of medicines. Am J Health Syst Pharm. 2009; 66(5 Suppl 3): S42-8 12
21 Leape LL, Bates DW, Cullen DJ et al. (1995) Systems analysis of adverse drug events. ADE Prevention Study Group. JAMA; 274(1): 35-43.
22 Vincent C, Taylor-Adams S, Chapman EJ et al. (2000) How to investigate and analyse clinical incidents: clinical risk unit and association of litigation and risk management protocol. BMJ; 320(7237): 777-81.
23 Reason J (1995) Understanding adverse events: human factors. Qual Health Care; 4(2): 80-9.
24 Dean B, Schaechter M, Vincent C, et al. (2002) Causes of prescribing errors in hospital inpatients: a prospective study. Lancet; 359(9315): 1373-8.
25 National Patient Safety Agency (2007)
26 Elliott M, Liu Y. (2010) The nine rights of medication administration: an overview. Br J NursMar 11-24;19(5):300-5.
27 Smeulers M, Verweij L, Maaskant JM, de Boer M, Krediet CT, Nieveen van Dijkum EJ, Vermeulen H. (2015) Quality indicators for safe medication preparation and administration: a systematic review. PLoS One. 2015 Apr 17;10(4):e0122695. doi: 10.1371
28 Taxis K, Barber N,(2003) Etnographic study of incidence and serverity of intravenoius drug errors.BMJ 326:684
29 Dean BS, Barner ND, (1999) A validated, reliable metohd of scoring the severity of medication errors. Am J Hosp Pharm 56 : 57-62
30 Gianino MM, Vallino A, Minniti D, Abbona F, Mineccia C, Silvaplana P, Zotti CM, (2007) A method to determie hospital costs associated with nosocomial infections. Ann lg 19(4) : 381-392
31 Bertolini G, Confalonieri M, Rossi; Simini B, Gorini M, Corrado A, (2005) Cost of the COPD. Differences between intensive care unit and respiratory intermediate care unit. Res Med 99: 894-900
32 Kohn L, Corrigan J, Donaldson M (2000) To Err Is Human: Building a Safer Health System. Washington, DC: Committee on Quality of Health Care in America, Institute of Medicine. National Academies Press, ISBN: 9780309068376
33 Ehsani J, Jackson T, Duckett S (2006) The incidence and cost of adverse events in Victorian hospitals 2003-2004. Med J Aust 184(11): 551-55 www.ncbi.nlm.nih.gov/pubmed/16768660
34 James JT A new, evidence-based estimate of patient harms associated with hospital care. J Patient Saf. 2013 Sep;9(3):122-8
35 Dehmel C, Braune S, Keymann G, Baehr M, Langebrake C, Hilgarth H, Nierhaus A, Dartsch D, Kluge S (2011) Do centrallly pre-pared solutions achieve more reliable drug concentrations than solutions prepared on the ward? Intensive Care Med 2010-00231. R3 in press
36 Tissot E. Cornette C, Limat S, Maourand J, Becker M, Etievent J et al. (2003) Observational study of potentioal risk factors of medication administration errors. J Qual Improve 25(6):264-68
37 Vogel Kahmann I, Bürki R et al. (2003) Incompatibility reactions in the intensive care unit. Five years after implementation of a simple "color code system". Anasthesist 52(5):409-12
38 Trissel LA (2011). Handbook on Injectable Drugs. 16th ed. Bethesda: American Society of Pharmacist.
39 Valentin A, Capuzzo M, Guidet B, Moreno R, Metnitz B, Bauer P et al. (2009). Errors in adminstration of parental drugs in intensive care units: multinational prospective study. BMJ 338:b814. doi:10.1136/bmj.b814
40 Taxis K (2005) Who is responsible for the safety of infusion devices? It's high time for action! QSHC 14(2):76
41 Rothschild JM, Keohane CA, Thompson S, Bates DW (2003) Intelligent Intravenous Infusion Pumps to improve Medication Administration Safety. AMIA Symposium Proceedings, p.992
42 Brigss J (2005) Strategies to reduce medication errors with reference to older adults. Best practice 9(4):1-6
43 Etchells E, Juurllink D, Levinson W (2008) Medication Errors: the human factor. CMAJ 178(1):63
44 Langebrake C, Hilgarth H (2010) Clinical pharmacists' interventions in a German University Hospital. Pharm World Svi 32(2):194-99
45 Kane-Gill SL, Jacobi J, Rothschild JM (2010) Adverse drug events in intensive care units: Risk factors, impact and the role of team care. Crit Care Med 38(6): 83-89
46 Jones JH, Treiber L (2010) When 5 rights Go Wrong. J Nurs Care Qual 25:240-247