Pain therapy in obstetrics
“Obstetric anaesthesia and analgesia is the only area of anaesthetic practice where two patients are cared for simultaneously.” > More information
Whenever an expectant mother receives pain treatment, an interdisciplinary team of physicians, nurses, and midwives takes care of two patients’ health – the mother and the unborn child. Adequate pain management in the field of obstetrics has undergone fundamental changes not only in the technique itself, but also in the understanding of medical outcome, related risks and the perception of pain.
In a perfect world differentiation between natural and elective birth would be sufficient whereas in reality unforeseen events could increase risk for both, the mother and her unborn child, potentially leading to an emergency. The health conditions mainly determines the suitable analgesia method and the decision between ‘vaginal vs. cesarean birth’. Additionally, factors like cultural background, expert advices and own expectations play an important role.
Modern pain management provides a holistic approach, starting from onset of labor, covering the phases of dilatation and expulsion and ending with treatment of a cesarean wound. Smart product solutions enable the pregnant woman to give birth in the most relaxing atmosphere with reduced or limited pain.
Prescription
Prescription
The appropriate approach to anesthesia and analgesia has to be decided based upon the clinical situation, planned procedure along with the patient’s conditions and preferences.
Local Anesthetics
Local Anesthetics (LA) prevent or relieve pain by interrupting nerve conduction. LAs can be divided into three categories: short acting (45-90 minutes), intermediate duration (90-180 minutes), and long acting (4-18 hours) and are mainly used for regional anesthesia techniques. The role of and demand for regional anesthesia will continue to grow as it has became evident that these techniques considerably improve patient outcome.
Related products - Prescription
Patient Access
Patient Access
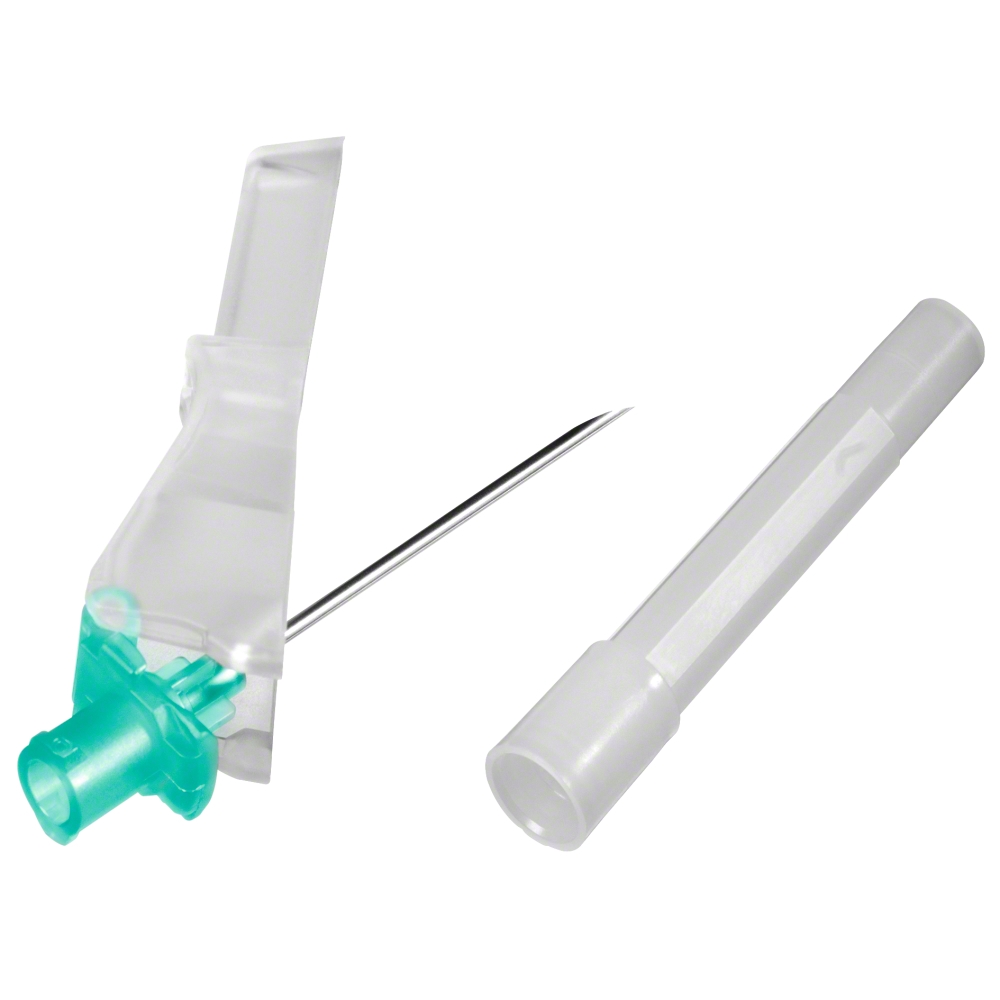
The patient access for anesthetic and analgesic therapies in the field of obstetrics depends on the method of choice: Neuraxial approaches require access to the vertebral canal in the appropriate layer (epidural or subarachnoidal space), whereas for general anesthesia using TIVA (total intravenous anesthesia) a venous access is mandatory.
In addition to the access paths, a peripheral venous access is indicated to manage supplementary infusion therapy and for potentially occurring emergencies.
More related products - Patient Access
Preparation
Preparation
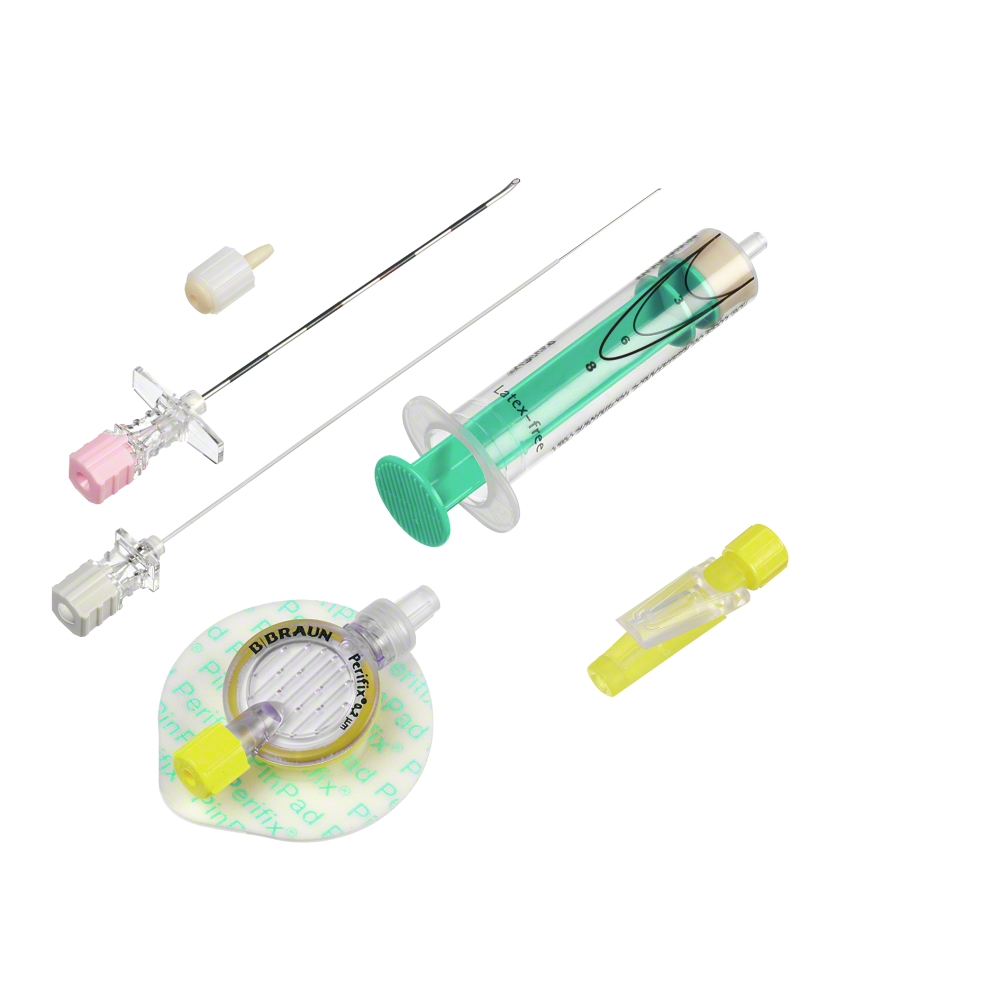
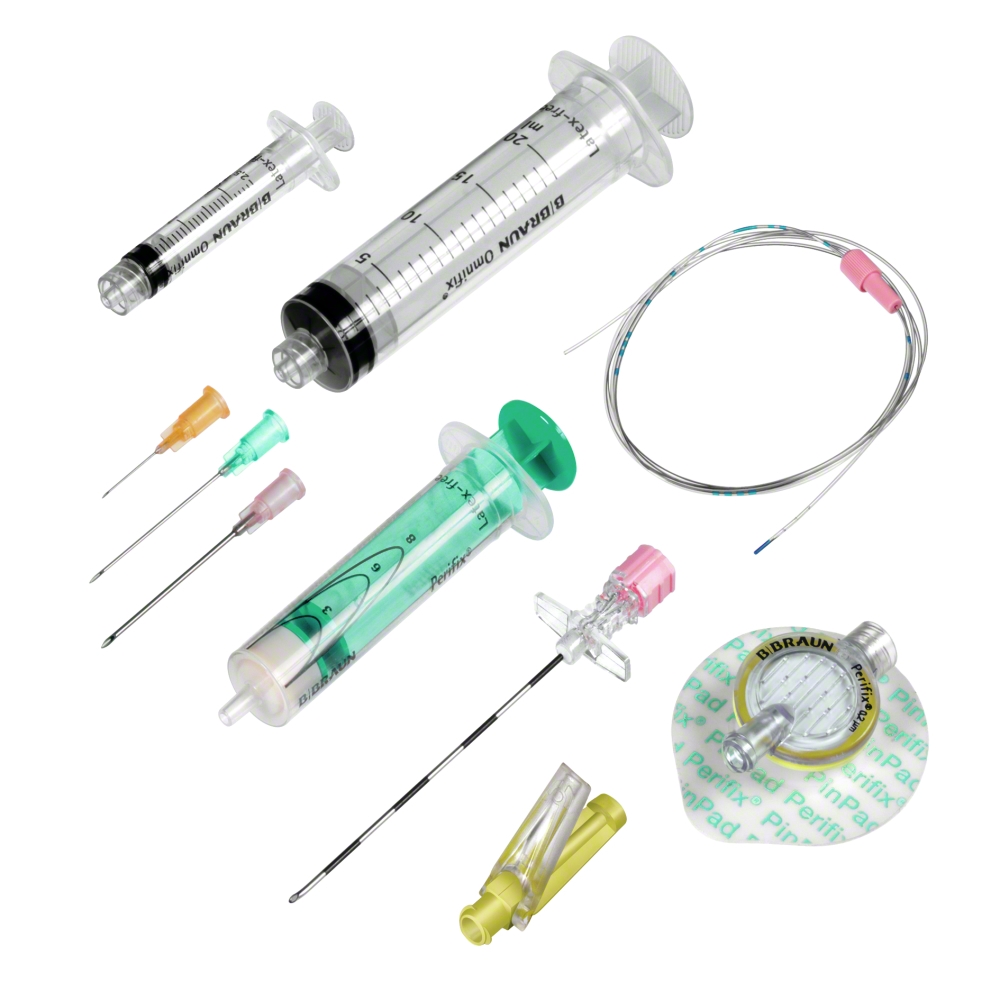
For preparation of the procedure, correct patient positioning is the prerequisite for a successful placement of neuraxial needles and catheters. Specific procedure kits containing all products required to perform the anesthetic procedure - from drapes over disinfectant to needle, catheter, connector and dressing - enable for a safer and efficient set-up.
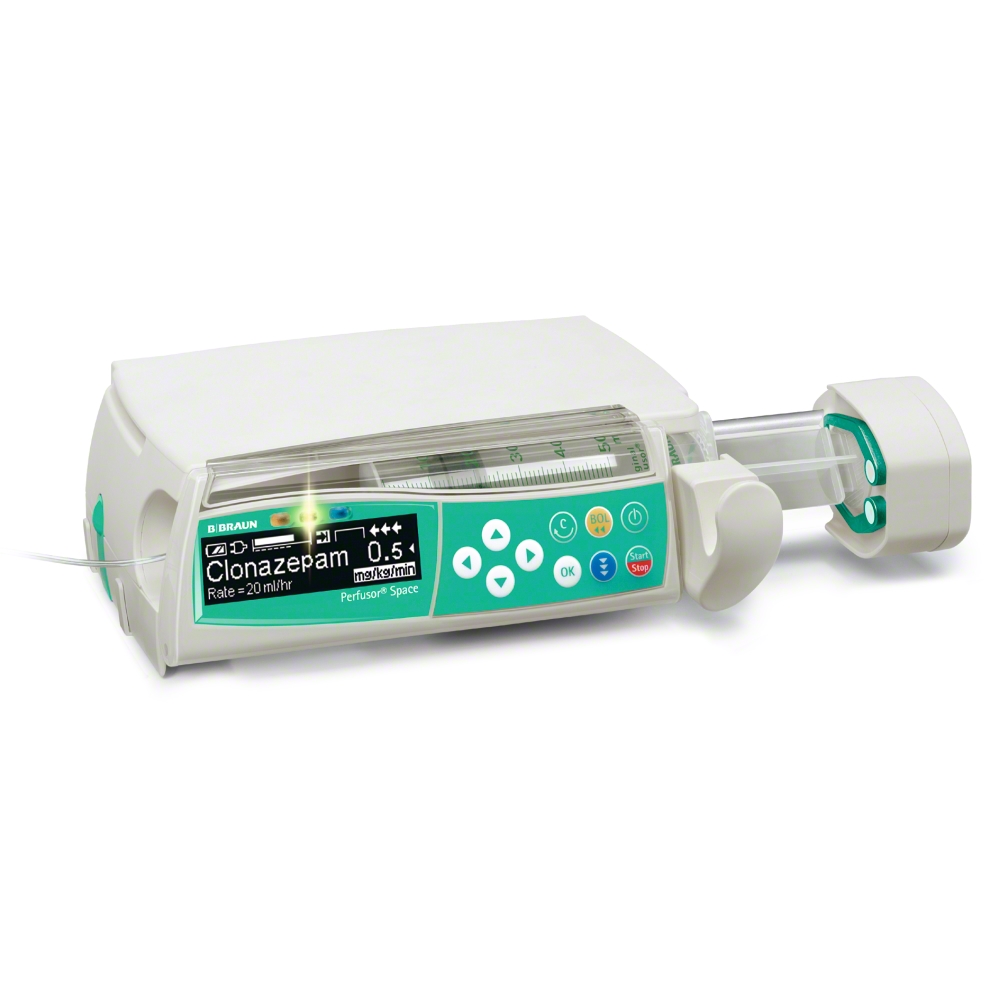
Continuous infusion, normally provided by the hospital pharmacy or prepared on ward, e.g. with a prefilled elastomeric pump, could be used for adequate pain management from labor onset until discharge management.
Application
Application
The application of anesthesia and analgesia largely depends on the selected approach: Neuraxial methods require the injection of the local anesthetic into the correctly positioned needle or catheter, either via a single-shot, intermittent bolus or a continuous infusion technique. Managing emergencies with TIVA as an anesthesia technique using smart pumps and algorithms for Target Controlled Infusion makes the application safer and easy.
Related products - Application
Discharge Management
Discharge Management
After giving birth, women would like to take care of their newborns. This should not be hindered by inadequate management of post operative pain, especially after a C-Section. Multimodal pain management in combination with new techniques, such as continuous wound infusion and peripheral nerve blocks (TAP block), increases comfort level during recovery.