Nutrition Therapy In Hospital or At Home
Nutrients for wellness
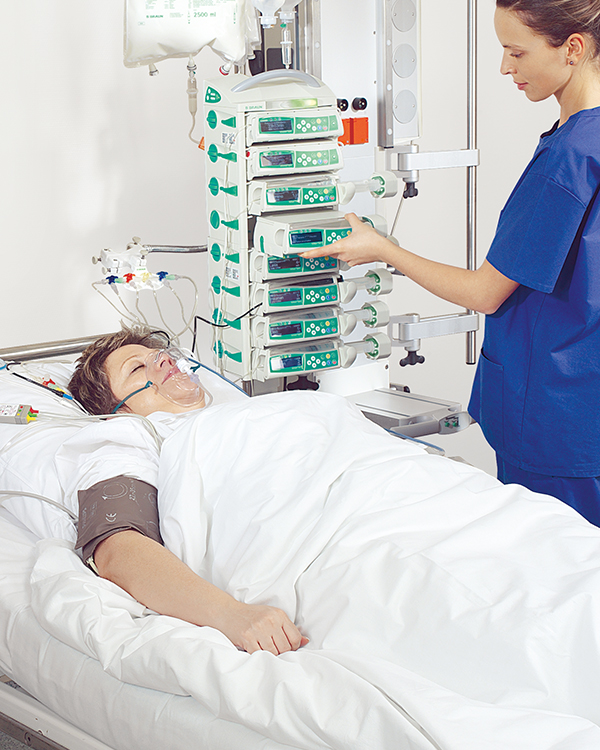
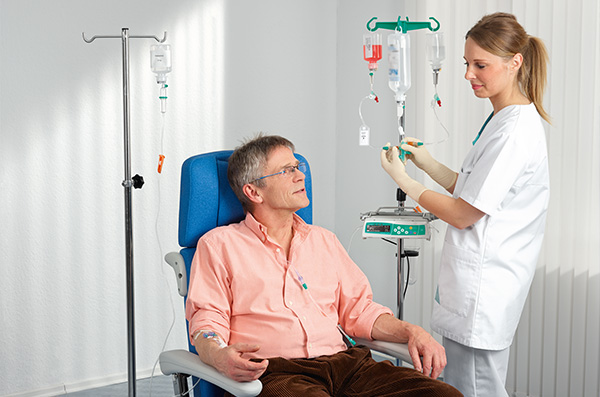
The Nutrition Therapy is of central importance for our ability to handle diseases in general, infections, surgery and trauma in particular. The objective of the Nutrition Therapy is to maintain or improve the nutrition status by avoiding and treatment of malnutrition, maintaining body tissue and functioning plasma protein stores and to prevent macro- and micronutrient deficiency.
Nutritional support can be provided either orally (oral nutritional supplements) or through a feeding tube (Enteral Nutrition) or, when the digestive tract cannot be used, through an intravenous catheter that is inserted directly into the veins (Parenteral Nutrition).
The definitive type of nutrition therapy is largely depending on the patients condition, illness and needs. E.g. surgical patients in an ICU tend to have needs different from those patients undergoing anti-cancer treatment or chronic dialysis yet again need another nutritional support.